How Hopper redefines patient access using Agentic AI—without sacrificing trust
When a patient calls an orthopedic clinic, they’re rarely calling about something simple.
They might be in pain. They might be post-operative and worried something’s wrong. Or they might be trying to navigate scheduling, billing, or next steps while already feeling overwhelmed.
For Chase Williams, SVP of IT Transformation at Hopper, that reality shapes everything.
Hopper is the largest value-based musculoskeletal (MSK) care organization in the United States, operating orthopedic clinics and partnering with providers nationwide to support patients across the full continuum of care, from the first appointment through recovery.
That responsibility demands systems that are as coordinated and connected as the care itself. For Chase, that starts with communication.
“Patients are inundated with messages today,” Chase explains. “But clinical communication has to be timely, meaningful, and easy. If it’s not, it breaks trust.”
The challenge: high expectations, low tolerance, and clinical risk
Healthcare communication doesn’t behave like communication in other industries.
Patients still want to call—especially when it comes to clinical care. Clinicians are already managing charts, lab results, orders, and multiple systems throughout the day. And tolerance for friction is low. A long hold, a few transfers, or a voicemail that goes unanswered can quickly turn into a poor patient experience.
As Hopper grew—bringing together clinics, joint ventures, and partners across the country—those challenges compounded.
“We want patients to make one call and get where they need to go as quickly as possible,” Chase says. “But without visibility, you don’t know where the experience is breaking—or how to fix it.”
Traditional telephony systems offered basic metrics, but not answers:
Did patients reach the right destination?
Were post-op risks being identified early?
How many transfers did it really take?
Where were workflows creating unnecessary delays?
Why Dialpad: A partner willing to learn healthcare
Hopper wasn’t looking for another phone system.
They’d seen too many platforms take legacy workflows, add the word “AI,” and call it innovation.
“What we needed was a partner willing to understand healthcare,” Chase says. “Healthcare runs differently—and for good reason. You can’t just drop technology in and hope it works.”
Dialpad stood out because of how the partnership worked.
From the beginning, Hopper and Dialpad worked side by side:
Reviewing healthcare-specific use cases
Meeting with clinicians and operational leaders
Feeding real clinical workflows into Dialpad’s roadmap
Iterating continuously, not annually
Even workflows many vendors consider outdated—like voicemail—were treated as critical.
“In clinical care, voicemail still matters,” Chase explains. “Prescription refills, post-op questions—those require clinician follow-up. Dialpad didn’t dismiss that. They invested in it.”
Reliability is foundational. When patients can’t get through, nothing else matters. Dialpad’s transparency around uptime and outages provided Hopper with the technical confidence to maintain high-stakes clinical environments.
Skipping IVR and going straight to conversational AI
Hopper ’s largest contact center in Phoenix—its “center of excellence”—became the proving ground.
Instead of moving incrementally from button-push interactive voice response (IVR) to speech recognition, Hopper made a deliberate decision: skip straight to conversational intake.
“We skipped speech and went straight to conversational,” Chase says. “We wanted the system to identify the goal quickly, confirm it, and execute.”
The approach was intentionally pragmatic:
Answer low-effort questions fast (hours, directions, addresses)
Detect post-op or risk language (pain, swelling, infection)
Route patients to the right destination immediately
Escalate to humans when needed—with urgency and context
Just as important, Hopper didn’t treat automation as the end goal.
“In healthcare, deflection isn’t always a good thing,” Chase explains. “Less call volume doesn’t necessarily mean better care. What matters is the outcome.”
Agentic AI became a way to support human judgment, not replace it.
From canned reports to real operational insight
The biggest shift wasn’t just how calls were handled—it was in the operational clarity. Hopper could finally see why patients were calling and where their access was breaking down.
Traditional telephony reports answer surface-level questions: call volume, answer speed, hang-ups. They don’t explain the patient experience.
With Dialpad’s AI capabilities—especially AI CSAT, AI Scorecards, and transcription analytics—Hopper gained visibility they’d never had before.
Instead of manually sampling a handful of calls, teams could analyze interactions at scale and focus on the moments that mattered most.
“We can now see where experiences are breaking down,” Chase says. “Not across the whole service—but in very specific parts of the patient journey.”
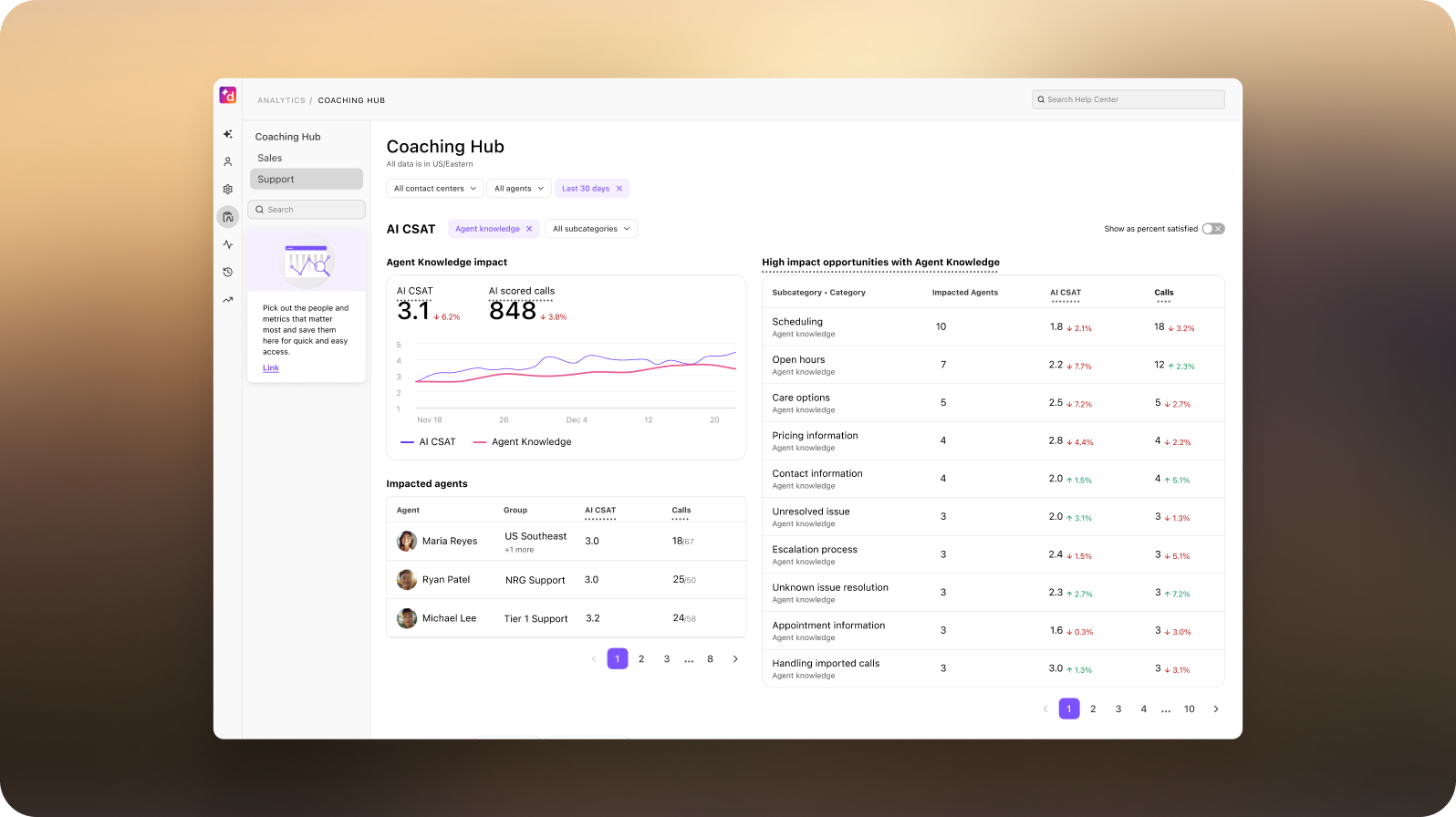
A real outcome: Transforming surgery scheduling
After the first Dialpad go-live at Hopper HQ and the Core Institute, one insight stood out quickly. Historically, surgery schedulers were assigned to individual clinicians, with limited visibility beyond appointment calendars.
Dialpad’s data revealed an opportunity to:
Cross-utilize scheduler resources
Specialize agents
Get patients to a scheduler faster
Help providers plan schedules more intelligently
“Before Dialpad, we didn’t have that level of insight,” Chase explains. “Now we do—and it directly improved the patient experience.”
Adoption in a clinician-first environment
Change in healthcare is hard—for good reason.
Clinicians have been inundated with technology for years, often without a clear explanation of why. Anything new can feel like friction.
Hopper took a deliberate approach:
Start small and purposeful
Explain the “why” in terms clinicians care about
Design workflows that reduce clicks instead of adding them
Be present at go-live to ensure clinical outcomes—not just technical success
“When clinicians understand the problem you’re solving,” Chase says, “the buy-in follows.”
A pragmatic vision for agentic AI in healthcare
Hopper doesn’t believe healthcare will ever be—or should be—100% automated. Patients need trust. Clinicians need accountability. AI needs guardrails.
“I don’t think AI should be binary—yes or no,” Chase says. “It should be supplemental. It should make you better at what you already do.”
For Hopper, success means:
Patients reaching the right destination faster
Clinicians calling back with full context
Risk being identified early
Operations improving without harming trust
Together, Hopper and Dialpad are building a repeatable model for healthcare communication—one that balances speed with safety, automation with humanity, and innovation with responsibility.
What’s next
Hopper sees healthcare communication at a crossroads. Patients still want to talk to people—but expectations for speed and clarity are higher than ever.
Working with Dialpad, Hopper is focused on:
Short time-to-value deployments
Targeted, safe AI use cases
Continuous improvement through analytics
Scalable solutions for healthcare organizations of all sizes
“Success for us,” Chase says, “is being able to look back and know we truly provided value—to our clinicians, our partners, and most importantly, our patients.”
Ready to build safer, smarter patient communication?
See how Dialpad’s AI-powered platform helps healthcare organizations modernize patient access—without sacrificing trust.



